Types of psoriasis
There are five main types of psoriasis:
Plaque psoriasis
Guttate psoriasis
Pustular psoriasis
Inverted psoriasis
Erythrodermic psoriasis
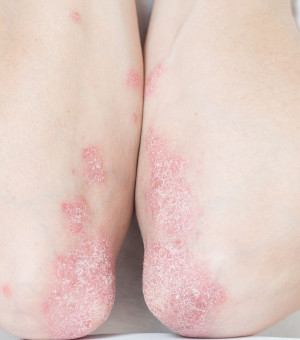
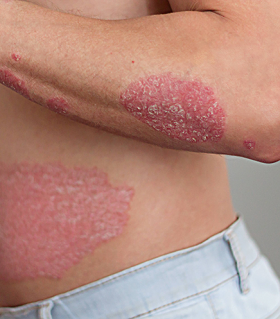
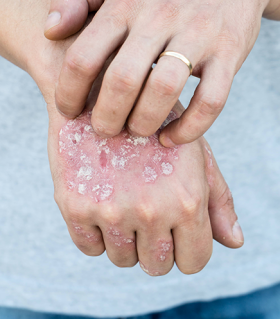
Plaque psoriasis
Plaque psoriasis (also known as psoriasis vulgaris) is the most common type of psoriasis, affecting about 90% of patients.
It appears as patches of inflamed skin, covered by an accumulation of skin cells that form a white, scaly layer called a squama.
Plaque psoriasis can develop on any part of the body, but most often occurs on the elbows, knees, scalp and trunk.
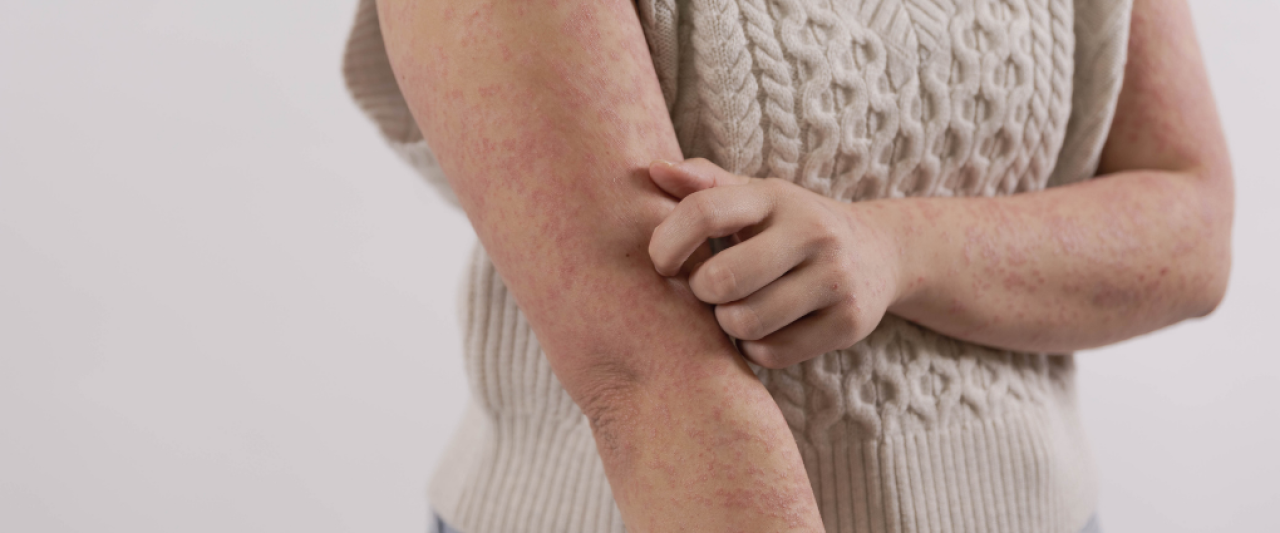
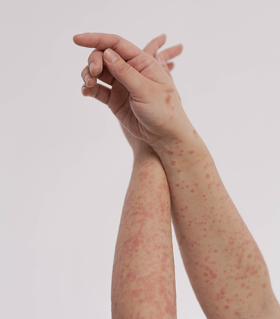
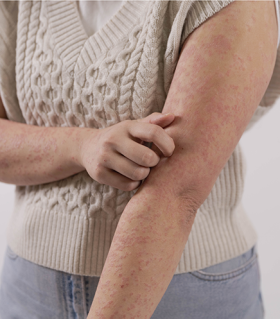
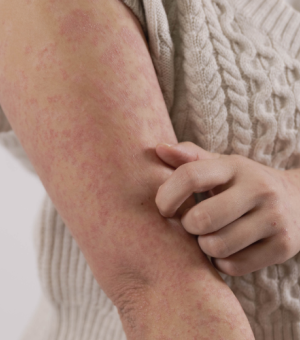
Guttate psoriasis
Guttate psoriasis comes from the Latin word gutta, which means "drop".
This form of psoriasis is characterised by small red, scaly patches of skin that often look like tears or raindrops. Hundreds of these small, drop-shaped patches can appear on the arms, legs, chest and sometimes the scalp. It usually affects children and young adults.
Although triggers vary, guttate psoriasis is strongly associated with strep throat and various sinus infections. If left untreated, guttate psoriasis can sometimes disappear on its own, or disappear and reappear as plaque psoriasis.
Inverse psoriasis
It is estimated that 21-30% of people with psoriasis suffer from inverted psoriasis (also called intertriginous psoriasis or flexural psoriasis). It occurs in areas such as the armpits, groin, under the breasts or buttocks, or any other area where the skin folds or bends. This type of psoriasis is characterised by smooth, inflamed lesions and may be moist to the touch. Inverse psoriasis lacks the scaling associated with plaque psoriasis due to the moist environment.
Inverse psoriasis is more commonly found in overweight or obese people, as they usually have excess skin and deeper folds. Symptoms of reverse psoriasis include irritation and itching and can be aggravated by rubbing or sweating. Loose, comfortable clothing is recommended, as it helps to avoid rubbing on the painful skin and prevents moisture from being trapped in the skin folds.
Pustular psoriasis
Pustular psoriasis is described as blister-like lesions filled with non-infectious pus and surrounded by reddened skin. It is a rare but severe type of psoriasis, usually seen in adults and often requiring immediate medical attention.
There are three different forms of pustular psoriasis: generalised, localised and acropustulosis.
Generalised pustular psoriasis is more severe, affecting larger areas of the body, and can develop suddenly and progress rapidly. Generalised pustular psoriasis can endanger the functioning of the kidneys and liver. Symptoms may include fever, chills, change in heart rate, muscle weakness and fatigue.
Erythrodermic psoriasis
Erythrodermic psoriasis is the rarest form of psoriasis, but also the most severe. It is estimated to affect 1-2% of people with psoriasis and is described as a skin-like rash over the entire body. It can cause intense itching or burning and usually spreads rapidly.
Psoriasis erythroderma interrupts the body's normal temperature and fluid balance, which can lead to episodes of chills and swelling due to fluid retention.
Most people with psoriasis have only one type of psoriasis, but some may have more than one type at a time or at different stages in their lives.