Saturday, August 20, 2022
Knowing the Difference Between Eczema and Psoriasis
Dr. Marc-André Doré

Sunday, February 13, 2022
Have you recently noticed that your baby has drier skin and a rash that seems to bother her? Could it be eczema? Do you wonder what you can do to help manage it?
In collaboration with Marie Fortier, a nurse specialised in pre- and post-natal care, we present a series of articles dedicated to the most common skin disorders in babies accompanied by our dermatologists’ advice. In this first article, we will shed some light on eczema.
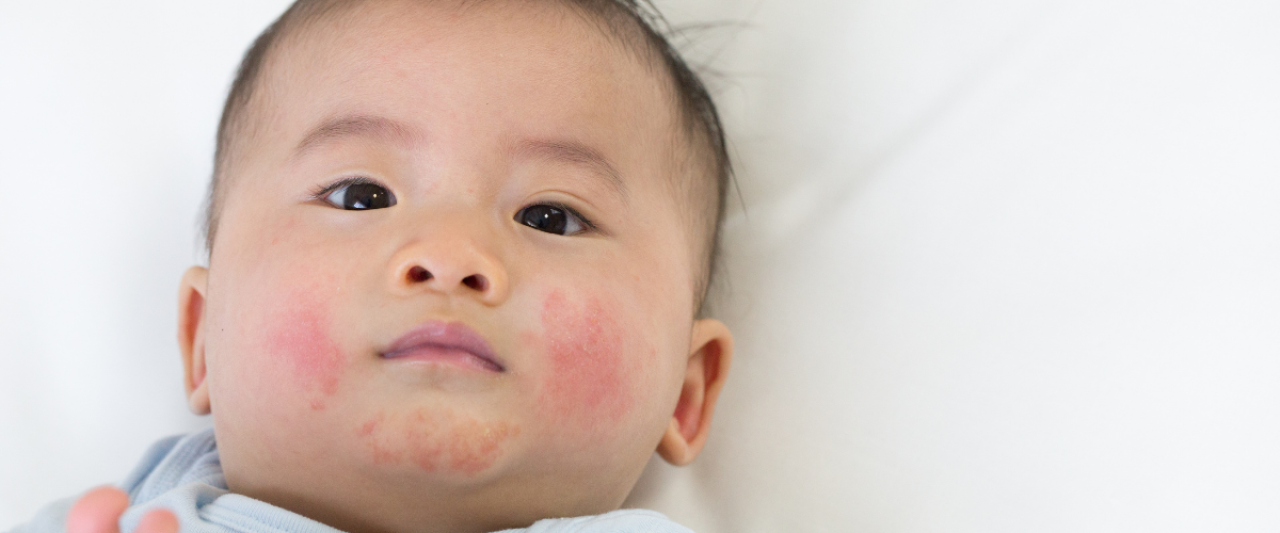
Eczema, or atopic dermatitis, is the most widespread chronic inflammatory skin disorder. Around one child out of six suffers from it. The first symptoms, such as red patches on the cheeks, may appear as early as 2-3 months. The rash may develop into a thickening of the skin and eventually a yellowish oozing crust may form.
Eczema can spread to the head, neck and forearms. The diaper area is usually free of eczema due to its humid environment. After the age of two, eczema patches will more commonly be found in the elbow and knee creases. The wrists, ankles, neck and area around the mouth are also likely to be affected. Typically, there will be flare-ups followed by symptom-free periods. Eczema is associated with a lot of itchiness and it is important to note that scratching will worsen the condition.

What is the cause?
The origin of atopic eczema is mostly genetic and implies a breakdown in the skin barrier. The skin is not able to retain water properly, which results in severe dryness and leads to hypersensitivity and skin breakdown. This will in turn provoke an immune and inflammatory reaction, hence the rashes and other symptoms. Bacteria on the skin’s surface can thereby be activated which can give rise to a local infection.
Eczema in children is frequently associated with other “atopic” disorders, such as asthma and seasonal allergies. It has been shown that a poor control of the symptoms of eczema early in life can increase the risk of suffering from asthma and allergies later. Consequently, it is important to manage the condition as early as possible.
In addition to prevention, SKIN HYDRATION is the key to managing the symptoms of eczema.

Give a lukewarm bath to your baby everyday (10 min max) to help moisturise the skin and get rid of bacteria (that could lead to infection, rash or secondary infection).
Use an unscented soap or cleansing oil for better skin hydration, for example Uriage Cleansing Oil, Cutibase Ceramyd Cleanser, Exomega Bath Oil.
Gently dry your baby by dabbing with a soft towel, without rubbing the skin.
Apply an unscented quality hydrating cream (moisturiser) on the whole body, even where there isn’t any rash or patches. Reapply cream several times a day if the skin is very dry.

Use a gentle and unscented laundry soap, for example Tide Zero. It is also advised not to use any fabric softener.
Loose-fitting clothes made of cotton or other smooth fabrics are the most appropriate for your baby. Wool and synthetic fibres are not advised. Ideally, use cotton sheets.
We want to avoid the child scratching as this could cause more skin damage and worsen eczema: it is a vicious cycle!

Regularly cut your baby’s fingernails to prevent scratching. Baby mittens at night time or even during the day can be a solution.
Spray skin lesions with mineral water to relieve itching. In the presence of extensive eczema, it is often necessary to administer an anti-itching syrup.
If the situation doesn’t improve, you will have to consult with a doctor to obtain appropriate treatment. A corticosteroid-based cream, which is not dangerous for your child’s skin, is often prescribed to gain control of the condition. Many treatment options are available.
According to some studies, a long breastfeeding period could help prevent eczema in babies with a genetic predisposition.
Eczema can arise between two months and two years-old but very rarely after the age of five.
A child who developed eczema at a young age has around a 60% chance to be eczema-free after the age of 12.
Generally speaking, eczema is not associated with food. There is sometimes an increase in rashes and itching when the child eats acidic food, such as tomatoes and strawberries, but this is not a food allergy.
This article is adapted from a post written in collaboration with Marie Fortier (French only).
For any question related to your personal situation, you can ask advice from our certified dermatologists at dermago.ca.
Looking to learn more?
Saturday, August 20, 2022
Dr. Marc-André Doré

Wednesday, June 22, 2022

Friday, February 18, 2022
Dr. Marc-André Doré
